FAQs
1. Can sleeping position influence the frequency of apnea events?
Yes. Many patients experience positional obstructive sleep apnea, in which apnea events occur more frequently while sleeping on the back. In the supine position, gravity pulls the tongue and soft tissues toward the pharyngeal wall, thereby narrowing the airway. Side sleeping reduces this effect, and this way airway collapse becomes less likely.
2. What role does genetics play in developing sleep apnea?
Genetics can influence several anatomical and physiological traits linked to sleep apnea. Inherited features such as a narrow jaw, enlarged tonsils, or a naturally restricted airway may increase collapse risk. Additionally, genetic differences in respiratory control stability can make certain individuals more susceptible to central sleep apnea.
3. Are there links between chronic nasal congestion and sleep apnea?
Yes. Chronic nasal obstruction increases airway resistance during breathing. As a result, the body must generate stronger negative pressure to inhale. This suction effect pulls soft tissues inward, thereby increasing the likelihood of pharyngeal collapse during sleep and worsening existing obstructive sleep apnea tendencies.
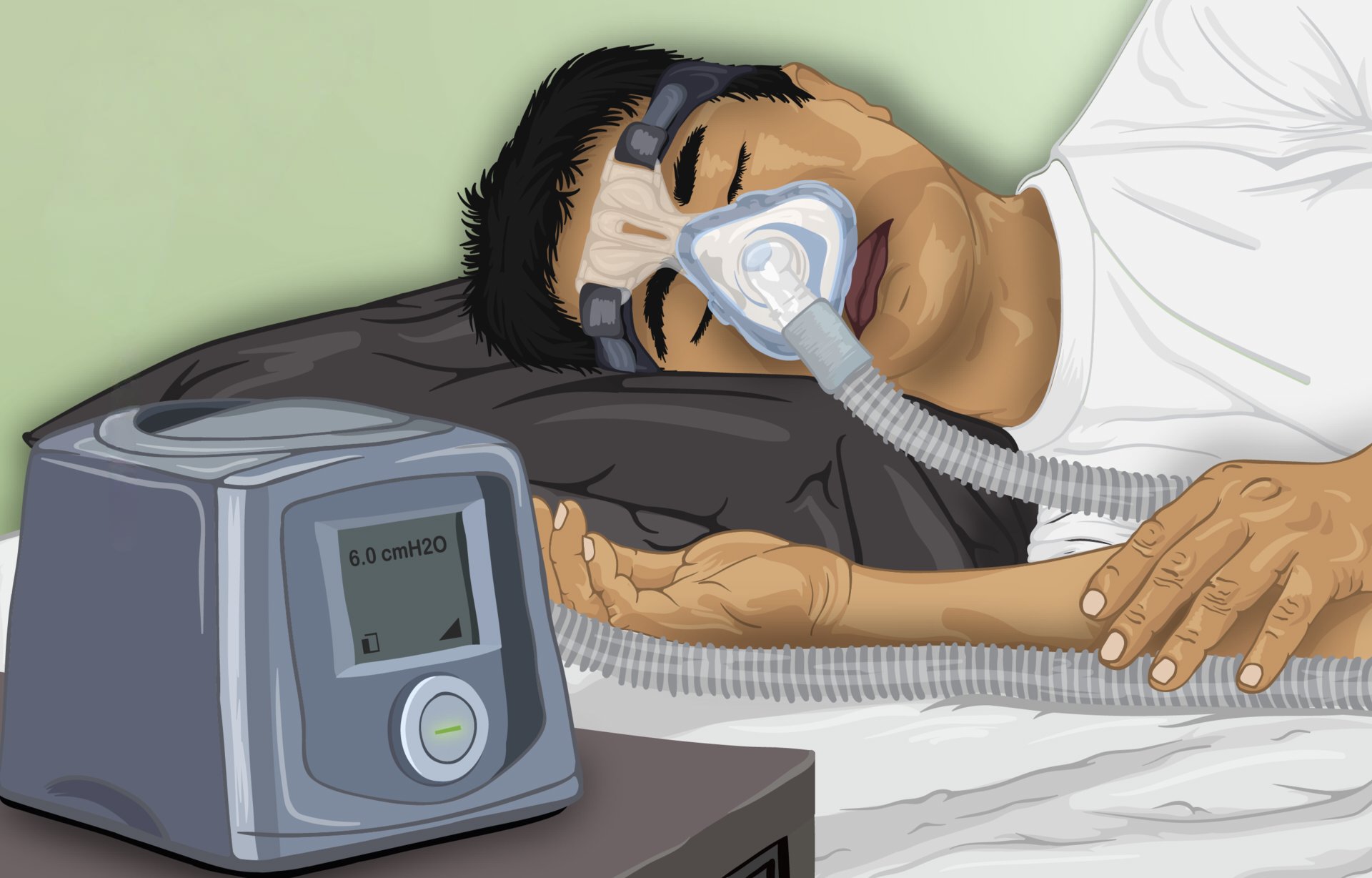
Image Credit: Original image from myUpchar via Wikimedia Commons. Edited to remove the text label on the instrument. Licensed under CC BY-SA 4.0.
Reference
1. Alakörkkö, I., Törmälehto, S., Leppänen, T., et al. (2023). The economic cost of obstructive sleep apnea: a systematic review. Sleep medicine reviews, 72, 101854.
2. Unnikrishnan, D., Jun, J., & Polotsky, V. (2015). Inflammation in sleep apnea: an update. Reviews in Endocrine and Metabolic Disorders, 16(1), 25-34.
3. Horner, R. L. (2012). Neural control of the upper airway: integrative physiological mechanisms and relevance for sleep disordered breathing. Comprehensive Physiology, 2(1), 479-535.
4. Owens, R. L., Eckert, D. J., Yeh, S. Y., et al. (2008). Upper airway function in the pathogenesis of obstructive sleep apnea: a review of the current literature. Current opinion in pulmonary medicine, 14(6), 519-524.
5. Aurora, R. N., & Punjabi, N. M. (2007). Sleep apnea and metabolic dysfunction: cause or co-relation?. Sleep medicine clinics, 2(2), 237-250.
6. Osman, A. M., Carter, S. G., Carberry, J. C., et al. (2018). Obstructive sleep apnea: current perspectives. Nature and science of sleep, 21-34.
7. Lyons, M. M., Bhatt, N. Y., Pack, A. I., et al. (2020). Global burden of sleep‐disordered breathing and its implications. Respirology, 25(7), 690-702.
8. Baillieul, S., Revol, B., Jullian-Desayes, I., et al. (2019). Diagnosis and management of central sleep apnea syndrome. Expert review of respiratory medicine, 13(6), 545-557.
9. Wellman, A., Genta, P. R., Owens, R. L., et al. (2014). Test of the Starling resistor model in the human upper airway during sleep. Journal of applied physiology, 117(12), 1478-1485.
10. Lv, R., Liu, X., Zhang, Y., et al. (2023). Pathophysiological mechanisms and therapeutic approaches in obstructive sleep apnea syndrome. Signal transduction and targeted therapy, 8(1), 218.
11. Javaheri, S. H. A. H. R. O. K. H., & Dempsey, J. A. (2013). Central sleep apnea. Comprehensive Physiology, 3(1), 141-163.
12. Antonaglia, C., Citton, G. M., Soave, S., et al. (2024). Deciphering loop gain complexity: a primer for understanding a pathophysiological trait of obstructive sleep apnea patients. Respiratory Medicine, 234, 107820.
13. Orr, J. E., Malhotra, A., & Sands, S. A. (2017). Pathogenesis of central and complex sleep apnoea. Respirology, 22(1), 43-52.
14. Cori, J. M., O’Donoghue, F. J., & Jordan, A. S. (2018). Sleeping tongue: current perspectives of genioglossus control in healthy individuals and patients with obstructive sleep apnea. Nature and science of sleep, 169-179.
15. Baptista, P. M., Costantino, A., Moffa, A., et al. (2020). Hypoglossal nerve stimulation in the treatment of obstructive sleep apnea: patient selection and new perspectives. Nature and science of sleep, 151-159.
16. Nigro, C. A., Dibur, E., Borsini, E., et al. (2018). The influence of gender on symptoms associated with obstructive sleep apnea. Sleep and Breathing, 22(3), 683-693.
17. Wimms, A., Woehrle, H., Ketheeswaran, S., et al. (2016). Obstructive sleep apnea in women: specific issues and interventions. BioMed research international, 2016(1), 1764837.
18. Franco, I., Reis, R., Ferreira, D., et al. (2016). The impact of neck and abdominal fat accumulation on the pathogenesis of obstructive sleep apnea. Revista Portuguesa de Pneumologia (English Edition), 22(4), 240-242.
19. Jun, J. C., & Polotsky, V. Y. (2016). Stressful sleep. The European respiratory journal, 47(2), 366.
20. St Louis, E. K. (2010). Diagnosing and treating co-morbid sleep apnea in neurological disorders. Practical neurology (Fort Washington, Pa.), 9(4), 26.
21. Xu, S., Wan, Y., Xu, M., et al. (2015). The association between obstructive sleep apnea and metabolic syndrome: a systematic review and meta-analysis. BMC pulmonary medicine, 15(1), 105.
22. Han, K. S., Kim, L., & Shim, I. (2012). Stress and sleep disorder. Experimental neurobiology, 21(4), 141.
23. Chopra, S., Rathore, A., Younas, H., et al. (2017). Obstructive Sleep Apnea Dynamically Increases Nocturnal Plasma Free Fatty Acids, Glucose, and Cortisol During Sleep. The Journal of Clinical Endocrinology and Metabolism, 102(9), 3172.
24. Muraki, I., Wada, H., & Tanigawa, T. (2018). Sleep apnea and type 2 diabetes. Journal of diabetes investigation, 9(5), 991-997.
25. Santiago, K. H., López–López, A. L., Sánchez-Muñoz, F., et al. (2021). Sleep deprivation induces oxidative stress in the liver and pancreas in young and aging rats. Heliyon, 7(3).
26. Malhotra, A., Grunstein, R. R., Fietze, I., et al. (2024). Tirzepatide for the treatment of obstructive sleep apnea and obesity. New England Journal of Medicine, 391(13), 1193-1205.
27. Spilsbury, J. C., Storfer-Isser, A., Rosen, C. L., et al. (2015). Remission and Incidence of Obstructive Sleep Apnea from Middle Childhood to Late Adolescence. Sleep, 38(1), 23.
28. Zancanella, E., do Prado, L. F., de Carvalho, L. B., et al. (2022). Home sleep apnea testing: an accuracy study. Sleep and Breathing, 26(1), 117-123.
29. Brennan, H. L., & Kirby, S. D. (2023). The role of artificial intelligence in the treatment of obstructive sleep apnea. Journal of Otolaryngology-Head & Neck Surgery, 52(1), s40463-023.
30. Gross-Isselmann, J. A., Eggert, T., Wildenauer, A., et al. (2024). Validation of the Sleepiz One+ as a radar-based sensor for contactless diagnosis of sleep apnea. Sleep and Breathing, 28(4), 1691-1699.
31. e Cruz, M. M., Chen, E., Zhou, Y., et al. (2025). A wearable ring oximeter for detection of sleep disordered breathing. Respiratory Medicine, 242, 108092.
32. Kwon, S., Kim, H. S., Kwon, K., et al. (2023). At-home wireless sleep monitoring patches for the clinical assessment of sleep quality and sleep apnea. Science Advances, 9(21), eadg9671.
33. Honda, S., Hara, H., Arie, T., et al. (2022). A wearable, flexible sensor for real-time, home monitoring of sleep apnea. Iscience, 25(4).
34. Sutherland, K., Vanderveken, O. M., Tsuda, H., et al. (2014). Oral appliance treatment for obstructive sleep apnea: an update. Journal of Clinical Sleep Medicine, 10(2), 215-227.
35. Goodday, R. H., Bourque, S. E., & Edwards, P. B. (2016). Objective and subjective outcomes following maxillomandibular advancement surgery for treatment of patients with extremely severe obstructive sleep apnea (apnea-hypopnea index> 100). Journal of Oral and Maxillofacial Surgery, 74(3), 583-589.
36. Nokes, B., Baptista, P. M., de Apodaca, P. M. R., et al. (2023). Transoral awake state neuromuscular electrical stimulation therapy for mild obstructive sleep apnea. Sleep and Breathing, 27(2), 527-534.
37. Bisogni, V., Pengo, M. F., De Vito, A., et al. (2017). Electrical stimulation for the treatment of obstructive sleep apnoea: a review of the evidence. Expert review of respiratory medicine, 11(9), 711-720.